A lasting memory of the coronavirus pandemic will be the weekly applause of families standing at their front door to show appreciation of the NHS during lockdown. Our love affair with the health service has never been stronger. But can the NHS achieve the digital transformation it needs to deliver excellent care and retain public support?
Even the NHS’s most committed supporters were probably surprised by the speed at which it was able to transform itself to be ready for the first wave of coronavirus. New Nightingale hospitals were built in days and many existing NHS hospitals were completely reconfigured.
Change that might previously have taken several years in the health services was implemented at speed and without resistance. This was a major factor in ensuring hospitals were not overwhelmed by the virus and that many lives were saved.
How the pandemic spurred structural change
For example, at Barking, Havering and Redbridge University Hospitals NHS Trust in Essex, 20 wards were transformed to care for COVID-19 patients, with a five-fold increase in critical-care capacity. Almost 6,000 patient appointments were held over the phone in April alone, reducing the need for people to come to hospital. Tony Chambers, chief executive, described it as “an incredible transformation”.
Similar stories are told of hospitals around the country. But as the UK begins to adjust for life after the pandemic, will this spirit of transformation survive beyond COVID-19? Chris Hopson, chief executive of NHS Providers, believes it will. “Hospital trust leaders feel they’ve been given permission to get on with things in a way they haven’t been before,” he says.
Hospital trust leaders feel they’ve been given permission to get on with things in a way they haven’t been before
There is widespread agreement that change is overdue in health and social care. The challenge is to find consensus for what NHS England should look like in ten or twenty years and how it should be paid for. Should change be mandated from the top and driven by the Westminster government or should local NHS leaders be empowered to create systems tailored to their own communities? One thing seems certain: privatisation is off the agenda, for the time being at least.
Digital critical for NHS long-term plans
Beyond the NHS organisational structure, digital transformation holds the key to a sustainable, publicly-funded health service. Slow adoption of digital technologies has been a major obstacle in the delivery of NHS long-term plans. Some of this is down to funding priorities. But there are also structural and cultural barriers in an organisation that still had more than 8,000 fax machines in 2019 and has only recently banned them.
Digital transformation has long been seen as critical in GP practices, which have struggled to cope with increased demand for services. But persuading patients, and some doctors, to use online consultations has been a major challenge. During COVID-19, almost all GP appointments have taken place online or by phone.
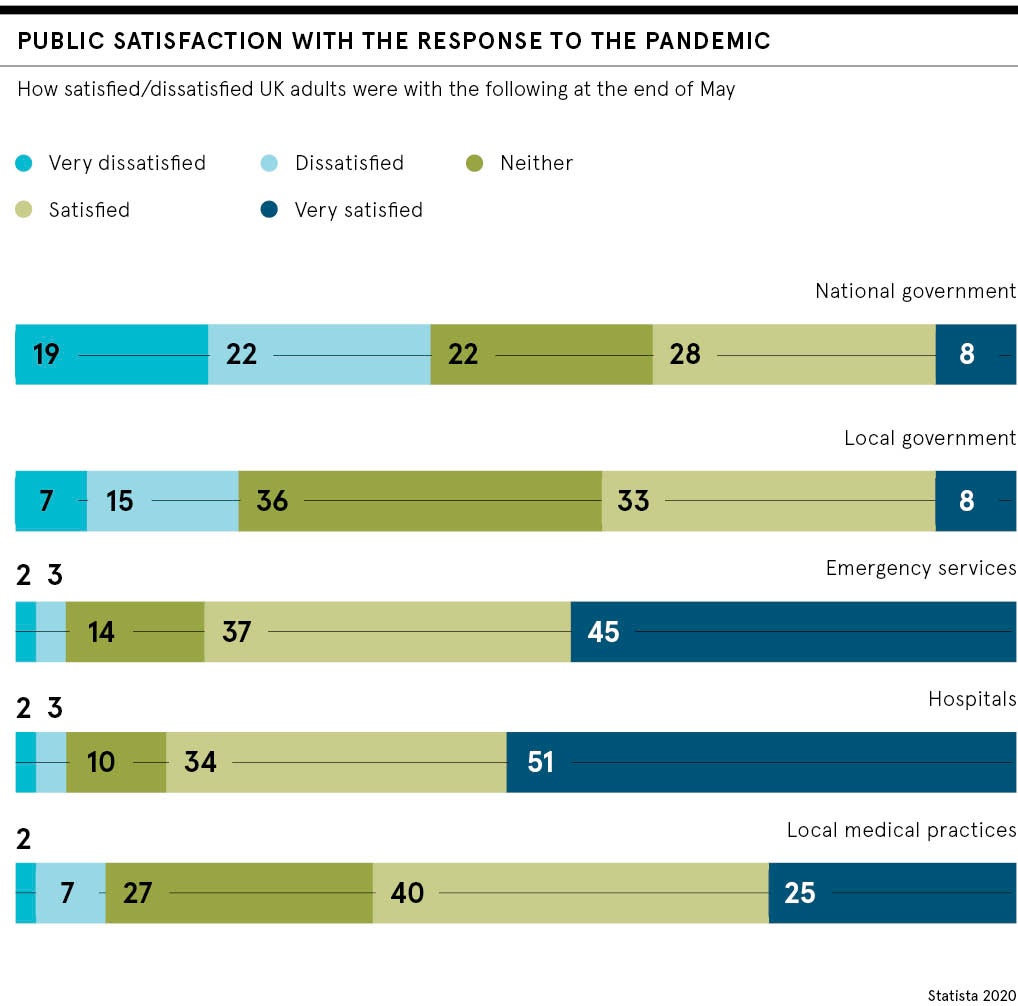
Health and social care secretary Matt Hancock has suggested that in the long term more than half of GP consultations could take place remotely. Yet NHS Digital’s own research shows that patients still overwhelmingly prefer face-to-face consultation and would like to return to old ways after the pandemic.
Amid concern that it could take four years for waiting lists to return to normal, NHS trusts have become emboldened to put forward ambitious plans for change which would have been unthinkable just a few months ago.
COVID-19 has sped up long-awaited change
Take the NHS in London, for example. After years of much discussion about change, but relatively little action, health chiefs in the capital are now planning to shift fundamentally the way healthcare is delivered in the wake of COVID-19. “It is critical that London enables a continuation of the culture of pace,” says Sir David Sloman, NHS regional director for London. “This means accepting a different kind of risk appetite than the one we are used to.”
The plan includes a new NHS organisational structure in London, with greater integration of health services, a permanent increase in critical capacity and remote delivery of more services. This is likely to be done at speed, with a new system in place from November 2021. To achieve this requires a level of digital maturity not often associated with an NHS organisation.
The government is also looking at ways to ensure the appetite for change and reform in the NHS is not lost and in so doing making sure it has greater control over additional billions of pounds of funding it has promised to the health service.
Mental health to benefit from digital transformation
This includes a plan to beef up what are known as integrated care systems (ICSs), informal groupings of NHS trusts, providing acute, community, mental health, specialist and ambulance services. They could be given formal legal status and put in charge of budgets with billions of pounds. The ambition is ICSs would tackle workforce, financial and waiting-time problems at a regional level, rather than leaving individual trusts to each do their own thing.
Of course, change will come at a cost. In the short term, NHS England will continue to draw on the chancellor’s blank cheque. The NHS cannot be caught out by a second wave of COVID-19 and there is also great pressure to alleviate waiting lists, particularly around cancer care, while maintaining infection controls. For the same reason, the NHS is redoubling efforts to move care out of hospitals and into the community, something that has been promised for many years.
But in the longer term, NHS England will need to demonstrate change brings real financial benefits to the taxpayer, as well as improving patient care, and this cannot happen without digital transformation.
How the pandemic spurred structural change
Digital critical for NHS long-term plans

