
Care workers earned our admiration and gratitude for the way they responded to the coronavirus emergency, often putting their own lives at risk to protect our loved ones. The pandemic laid out in stark relief just how critical social care is to communities, to the economy and to the NHS.
But the harsh reality is that working in health and social care is still seen as unappealing. The care sector entered the pandemic in a difficult position, with acute staff shortages, poor working conditions, low morale and a lack of investment in buildings and technology.
The COVID-19 death toll in care homes was shocking. The question is whether the pandemic will bring stakeholders together with a new sense of urgency to address these deep-rooted issues.
The future of the care sector is shrouded in uncertainty by repeated delays to social care reforms, including the way in which it is funded. Related to this are the financial problems of many of the private providers in the care sector. A number of the biggest care home companies require financial reconstruction while many family-run businesses are struggling to stay afloat.
While the NHS has experienced significant staffing pressures, the issues in social care are even greater and the outlook is a concern. One measure of the workforce supply gap is the vacancy rate. This rose from 5.5 per cent in 2012-13 to 7.8 per cent in 2018-19. In London it was 9.3 per cent, making it the region with the highest rate. The number of vacancies in social care in England is estimated to average 122,000 at any one time.
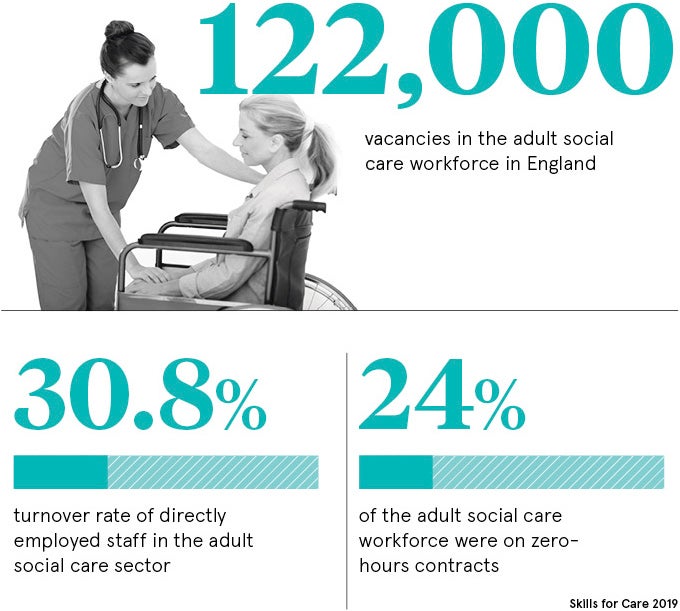
Supporting vulnerable people increasingly hard
Staff shortages have been exacerbated by uncertainties over Brexit, with many care workers in the UK originally from European Union countries and unsure about their future status, which makes working in health and social care even more precarious.
Measuring the full impact is difficult because of the disruption to travel caused by the pandemic, but the sector remains sufficiently alarmed to press the government for urgent clarification about what will be done to ensure the elderly and vulnerable people are not left without good care because of the deepening skills shortage. Unison, the union, has called for an urgent review of pay and conditions in the social care sector.
One of the lessons of the pandemic has been the extent of mutual dependence between the NHS and social care. When the care sector fails, the NHS is put under additional pressure and vice versa.
The NHS Long Term Plan for England, published last year, puts significant emphasis on supporting more people in the community. But this is only possible if people are willing to work in the health and social care sector, supported with the training and the technology they need.
This is not just about how we look after people as they become older and frailer, but about people of all ages who live with long-term conditions that require care and support. And it is about mental health as well as physical health.
Joined-up health and social care is vital
Technology can provide some of the answers. Since COVID-19, healthcare organisations have been moving services online at a dramatic pace. The most obvious impact has been to reduce the number of physical visits to the GP and hospitals. But behind the scenes, digital tools have been used to bring different services together across primary care, community services, hospital services and social care to work together to deliver joined-up care.
Innovative technologies have also enabled teamworking among much broader networks involving family members, peers and local communities, allowing parents to monitor their children’s health while at school or patients to create support communities including their peers, volunteers and friends.
Clinical teams need new pathways and new ways of working if we are to deliver high-quality proactive care to our patients in this new world
The coronavirus outbreak has highlighted how woefully inadequate paper processes are for the care sector, particularly at a time when the risk is changing hour by hour. By digitalising care-planning processes and evidencing care using mobile technology, providers can make time efficiencies that empower carers. Not only can care evidencing apps save carers time, they also give them the tools they need to do their job. They provide reliable reminders, highlight concerns and enable carers to monitor residents’ wellbeing.
Icon-driven apps that evidence care at the point of care have been shown to save each carer up to an hour a day in paperwork. With almost 1.5 million people working in social care, such additional capacity would be transformational.
Tech alone is not enough
Better still, the insights generated by digital systems can create an environment of constant improvement by highlighting where provision needs to be developed, and identifying trends across all areas of resident wellbeing from sleep, nourishment, hydration and medication to exercise and mental stimulation.
But technology alone will not provide all the solutions. Systemic change is needed. Dr Matt Kearney, GP and programme director at UCLPartners, says: “Technology will be a key enabler, but clinical teams will need new pathways and new ways of working if we are to deliver high-quality proactive care to our patients with long-term conditions in this new world.”
Sally Warren, director of policy at the King’s Fund health and care think tank, concludes: “Too often, politicians of all parties decided they couldn’t afford the political capital and the financial cost of social care reform. We can only hope the current crisis is showing they can’t afford not to.”

Care workers earned our admiration and gratitude for the way they responded to the coronavirus emergency, often putting their own lives at risk to protect our loved ones. The pandemic laid out in stark relief just how critical social care is to communities, to the economy and to the NHS.
But the harsh reality is that working in health and social care is still seen as unappealing. The care sector entered the pandemic in a difficult position, with acute staff shortages, poor working conditions, low morale and a lack of investment in buildings and technology.
