Data can be the lifeblood of the NHS. As John Bell, regius professor of medicine at Oxford University, remarked in the government’s life sciences industrial strategy: “One of the most important resources held by the UK health system is the data generated by the 65 million people within it.”
However, collecting and securely distributing patient information is a global healthcare challenge. Medical data typically flows from many different directions, with records kept as a mishmash of electronic and paper files scanned to a computer.
 Obtaining patient consent to share data can be difficult, especially in the UK where many different physical legal entities operate under the NHS umbrella. And a lack of standardisation in note-taking is a major problem for interoperability across different workflows.
Obtaining patient consent to share data can be difficult, especially in the UK where many different physical legal entities operate under the NHS umbrella. And a lack of standardisation in note-taking is a major problem for interoperability across different workflows.
As a consequence, although it is improving, access to data for patients and clinicians is far from frictionless and can result in poor care.
A recent study by York, Manchester and Sheffield universities found that around 237 million medication errors are made in England annually, causing at least 1,700 hospital patient deaths. Mistakes often occur due to a lack of information or because of communication errors.
The rise in digital health solutions and the bourgeoning role of artificial intelligence in disease diagnosis and preventative care has put a renewed onus on data management and sharing, but finding the right tools is problematic.
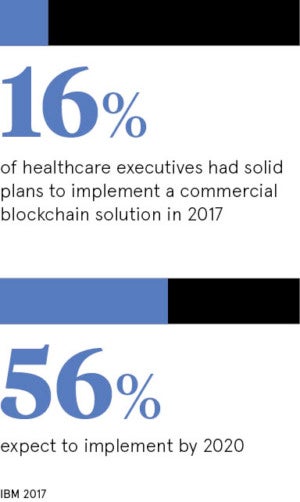
In the United States, which has an inexplicably complex healthcare system, some companies and organisations are looking to blockchain to manage this information.
Whenever records are accessed, this is shown in the blockchain, creating an immutable audit trail
American startup SimplyVital Health’s Connecting Care platform uses blockchain to facilitate sharing of patient records between providers from different clinical affiliations. The notes are not stored on the chain, but can be accessed from it. Whenever records are accessed, this is shown in the blockchain, creating an immutable audit trail.
Kat Kuzmeskas, the company’s chief executive and co-founder, says blockchain is good for transactions, immutability and security, but it is not good for storing chunks of data as it can’t hold enough, only mere megabytes, whereas one X-ray alone is several gigabytes.

Kat Kuzmeskas, chief executive and co founder of SimplyVital Health, says blockchain can open up access to data without having to turn it over to someone
“However, it can open up access to data without having to turn it over to someone,” says Ms Kuzmeskas. In America movement of medical records is a ‘business issue not a tech issue’, she adds, because to get paid, doctors need to prove they co-operated with other physicians in sharing information. Therefore, there is a clear incentive to create an audit trail of data-sharing.
MedRec, which is being developed at the Massachusetts Institute of Technology, further aims to link patients and providers to the addresses of existing remotely stored medical records using blockchain. Estonian-based Healthureum is targeting Indian healthcare with a similar platform that also securely consolidates medical data.
The US Center for Disease Control and Prevention is exploring the technology for public health surveillance, including using it to manage data more efficiently during a crisis. The centre thinks blockchain’s inherent security could be used to store and share data records faster during a pandemic, while complying with security and privacy laws.
Without the financial incentive, the use-cases for blockchain in UK healthcare seem less obvious. Yet Shaun O’Hanlon, a former GP and now chief medical officer at EMIS Group, a major provider of healthcare software services in the UK, believes it could be used as a record of patient consent.
“A major challenge for data protection is to make sure patients have given permission to access their data,” says Mr O’Hanlon. “An unconscious patient may arrive in A&E and doctors won’t know if they are allowed access to their medical records. Blockchain could be a way to define consent in one place with a proper audit trail.”
Furthermore, it could be used as a record for patient care to identify mistakes and liability. In 2016, the Royal College of Physicians found that tens of thousands of patients were having “do not resuscitate” orders imposed without consent.
“This requires an audit trail to make sure the doctor has recorded things properly and hasn’t changed or edited it,” says Mr O’Hanlon. “This is very important legally to protect the integrity of records and blockchain is ideal as we will know who recorded, accessed or deleted something.”
Blockchain is deemed secure because information submitted to the chain cannot be erased or edited and only people given permission can access the chain. The information stored, however, is distributed and some are actually concerned about the lack of a central administrator.
“Most people like the concept of a trusted central authority,” says Professor James Batchelor, director of the Clinical Informatics Research Unit at Southampton University. “As patient data is not stored in the chain, it becomes a mere reference to an individual, pointing to another system, so the point of principle is lost.”
He adds that it could solve problems in the future. “But as it stands now, I think it would be a struggle to implement and use it in any meaningful way,” says Professor Batchelor.
Blockchain technology is still nascent and there are problems with scalability. Transactions cost fractions of a penny, but the computing and electrical power needed is at present unsustainable at scale, according to Ms Kuzmeskas. However, she is confident this issue can be overcome, adding that the technology is essentially in the “dial-up stage”.
But, as Mr O’Hanlon concludes: “If there is a strong enough business case, it will happen eventually.” Although blockchain is almost certain to take off in private healthcare and the most modern systems first.


