For generations, cancer was known as the “Big C”, a disease so frightening and deadly that sufferers could barely utter its name. But scientists believe the next generation of patients may start to have a very different experience of cancer.
Peter Johnson, chief clinician at Cancer Research UK, says: “In some cases, cancer will become a chronic disease rather than a killer. This is already happening in diseases such as breast cancer and with the new molecular therapies. But at the same time we are looking for treatments to cure patients completely.”
New treatments and better survival rates for some cancers have already started to shift patient behaviour, Professor Johnson says.
“Patients used to think nothing could be done and so were reluctant to see a doctor quickly. But the message is starting to get through that getting diagnosed early will make a big difference to the chance of surviving cancer and we are seeing a change in attitude, with more people coming to the doctor sooner.
“A lot more still has to be done to encourage patients to get diagnosed sooner, but these sorts of shifts could have an important impact in the years to come.”
In future, the conversations between patient and doctor could change dramatically. At diagnosis, for example, patients will be given far more detail about their tumour based on molecular analysis carried out during an initial biopsy or blood test. Clinicians should be able to tell patients far more about how their cancer will behave and the types of treatments that will help.
“The process of diagnosis is going to be more sophisticated and also the types of treatment,” Professor Johnson says. “Keyhole surgery using robots will be far more common and this will minimise trauma to the patient, helping them to recover more quickly.
Clinical trial data reveals impressive, often extraordinary results, although important data showing whether these patients actually live longer is yet to come
“Radiotherapy will be more finely targeted to cause less damage to surrounding tissues, while proton beam therapy is another approach to treating cancers in difficult areas such as the brain. In addition to this, we are already using more targeted treatments and antibody treatments, with very exciting results from immunotherapy for melanoma and lung cancer.”
In an era of NHS cutbacks, important questions remain. For example, will health systems be able to afford the cost of the genetic tests and the new drugs that patients need? Or could the imminent arrival of new treatments be delayed by lengthy negotiations between industry and government over price?
Few health economists, think-tanks or charities seem ready to broach this controversial subject. Professor Johnson points out: “I think it’s important to recognise that cancer drugs are a small proportion of the total NHS budget.”
But away from the detail of who will pay for what, the new era of cancer treatments is getting tantalisingly close. Each month, clinical trial data is published revealing impressive, often extraordinary results, although important data showing whether these patients actually live longer is yet to come.
However, this has not stopped new drugs, known as immunotherapy checkpoint inhibitors, made my firms such as Bristol-Myers Squibb and Merck, from electrifying science journals and financial markets.
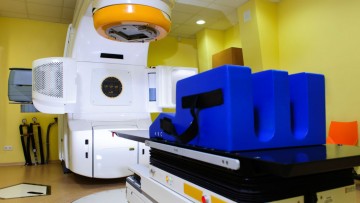
Cancer treatments such as radiotheraphy are becoming more targeted meaning they cause less damage to surrounding tissues
Tumour shrinkage in melanoma patients in a recent trial, prompted Dr Stephen Hodi, associate professor of medicine at the Dana-Farber Cancer Institute, to describe them as “simply unprecedented”, while another doctor said one patient’s dissolving tumour was “one of the most astonishing responses ever seen”.
Work using T cells from a patient’s own body to attack cancerous cells has also shown encouraging results in the treatment of leukemia, with some dying patients apparently cured using the approach.
In addition, scientists are excited by work using a patient’s own dendritic cells to create a vaccine, which can help to provoke the immune system to fight and kill cancer cells.
Almost all the pharmaceutical giants, including Novartis, Roche, Merck and AstraZeneca, are racing to get immunotherapies on to the market with trials focusing on various forms of cancer.
But recent results suggest the most promise will come not from using one drug, but from combining many types of immunotherapies including cancer vaccines. Knowing which combination to use and when could still take a long time for researchers and industry to unravel. And collaboration will again be needed provide the results that clinicians and patients need.
Navid Malik, an industry analyst and non-executive director of vaccine pioneers Northwest Biotherapeutics, says it’s not just pharmaceutical firms that hold the key to cancer breakthroughs.
People are too scared to say we’re on the verge of beating some cancers, but what’s coming around the corner is truly exciting
“Clinical trials have changed in recent years and are shorter and more focused these days,” he says. “This means that smaller biotechnology firms have the power to research and trial new cancer therapies too. This is the renaissance period for biotechs. Why do they need to work with pharmaceutical firms if they can get to market this fast?
“Up until recently, you could count innovation in cancer drugs on one hand but now, with immunotherapy and cancer vaccines showing impressive results in shorter trials, this is all changing.
“People are too scared to say we’re on the verge of beating some cancers, but what’s coming around the corner is truly exciting.”

