A changing society, characterised by the elderly living far from their children, dual-career families, some with financial challenges, is ratcheting up the strain on paid and unpaid carers as many people are now being asked to live at home with minimal care packages.
Dangers from falls, deteriorating health, loneliness and isolation can be addressed by technology, but such innovation has to be synchronised with effective service and support, says Gordon Sutherland, chief executive of market-leading Tunstall Healthcare.
The Yorkshire-based company, which has 60 years’ heritage pioneering technology to enable people to live at home independently, is taking its expertise to new levels to create highly effective models for care.
Building on its background of reactive response systems for social-care issues, it is helping to create new care systems that can help monitor chronic, long-term conditions and predict where and when help is needed. Its intelligence-driven capabilities are paving the way for more connected and predictive care.
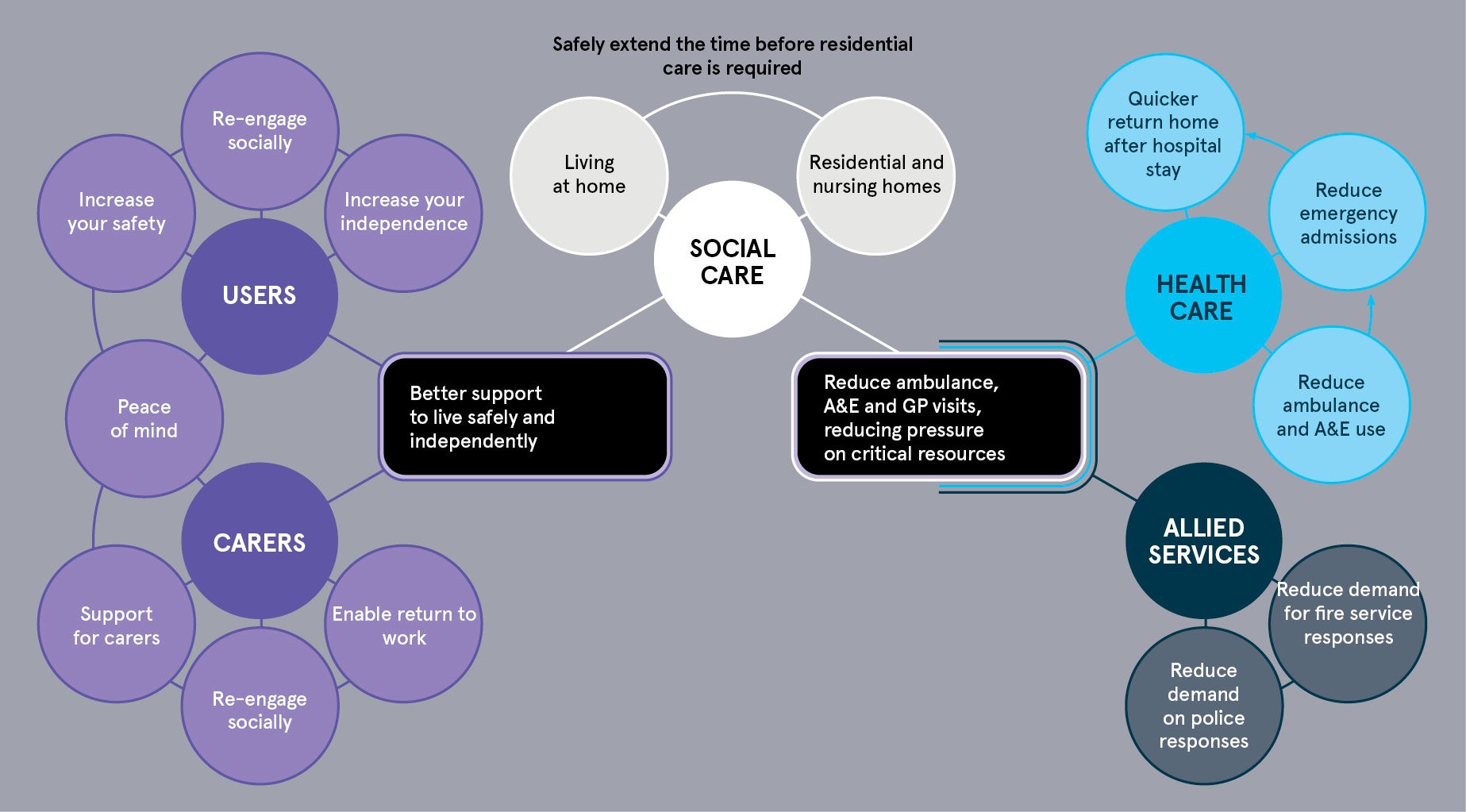
The Tunstall research programme has developed an integrated and quantified map of the resource benefits that are potentially realisable with Telehealth and Telecare. The research conclusively demonstrates how effectively managed and integrated telecare programmes can have a major impact in current operating terms. This includes savings of £4.5k per person per annum in social care costs for users who have telecare compared with those with similar needs but who do not have telecare. Preliminary evidence also points to potential benefits for healthcare and further research has been commissioned to consider these aspects definitively. However, even based on the capacity release in the social care system alone (i.e. additional costs avoided), the economics are
compelling.
“There is a great emphasis and expectation on technology being able to save the social-care system and we believe strongly in its potential,” says Sutherland. “But we need it to work in the community every day; it is more than delivering a shiny, new piece of technology. It is about finding a long-term, cost-effective solution.
“It is about innovation in the integration of healthcare and the social-care system that will make the technology work to its full potential. It is about being open to change the way we have traditionally delivered services.
“The integration of health and social care needs is critical. We can play a big part by enabling more people to live at home, or where they choose, for longer and help them and their families feel secure.”
Tunstall, which operates throughout Europe, the Middle East, China, Canada and Australasia, has seen its technology progress from the familiar red-button response system to the deployment of digital sensors and medical devices to analyse behaviour patterns and provide early warnings of failing health and also prediction of falls.
Developing systems where technology synchronises with GPs and hospitals has the potential to reduce unnecessary clinic and A&E visits and reduce strain on community nurses.
“We are transitioning from being the provider of just the technology and software to a company that collaborates with healthcare and social services to develop a ‘wrap-around monitoring, connectivity and data analysis’ system based on the data you, the citizen, want to share. This way it helps people to continue to live at home with a life they want,” says Sutherland.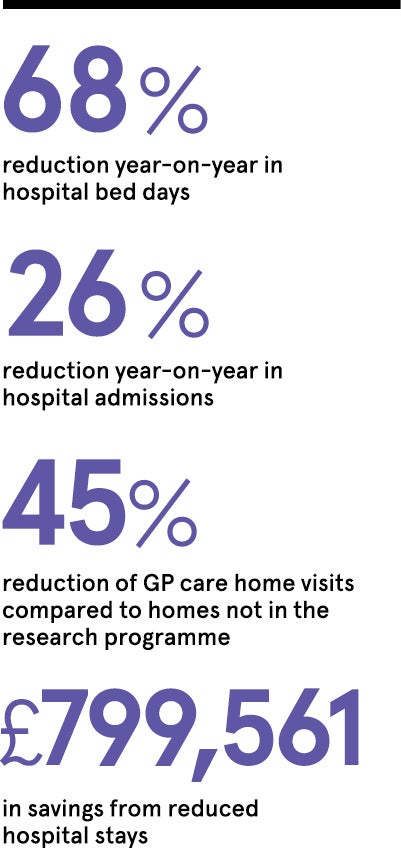
The importance of technology is echoed by the TEC Services Association, the representative body for technology-enabled care services. Chief executive Alyson Scurfield says connected health information and data will help deliver personalised care.
“We need to focus on improving the lives of people enabled by technology and shifting to outputs and outcomes for people,” she says. “Technology on its own will not solve any system, but service transformation and putting the service user at the heart of everything they design will.”
Tunstall is working with leading hospitals, government bodies, local authorities, universities and innovation centres across the UK and Europe to develop a new, advanced cognitive care system that utilises multiple smart devices, wearables and sensor technology for real-time messaging to clinical and social support as well as family members.
The aim is to provide core support, enhance and encourage healthy living and improved wellbeing while driving cost-efficiencies through financially constrained healthcare systems.
“Countries across Europe have adopted different approaches to manage this issue and there is a growing realisation of the overall benefits of investing in social healthcare and that technology can be a conduit to social engagement to offset the effect of exclusion or loneliness,” says Sutherland. “Technology can monitor for subtle changes in behaviour which may indicate or predict a fall, or the onset of a health concern.
“We are seeing exciting developments in a rapidly developing sector, but our vision remains constant: to help people have the freedom to live their life to the full in a place of their choice.”
For more information please visit www.tunstall.com



