The recently published ten-year plan for the NHS made a welcome commitment to increase spending on mental health by some £1.9 billion. This urgently needed funding will help to improve the care of people with mental illness, an area of healthcare that has always suffered from significant underinvestment compared with physical healthcare.
Currently, the UK has a revolving door of mental healthcare, whereby patients who are discharged from hospital are later readmitted due to a lack of available care in the community. This is failing patients and their families, the NHS and healthcare providers.
At Cygnet Health Care we take a considered, long-term approach to addressing mental illness and have pioneered a range of new services to treat our service users, though we recognise that all providers in the sector need to do more to ensure the best outcomes for patients.
We provide safe and comfortable mental health rehabilitation environments to help people rebuild their life and vocational skills, ready to regain their place in the community
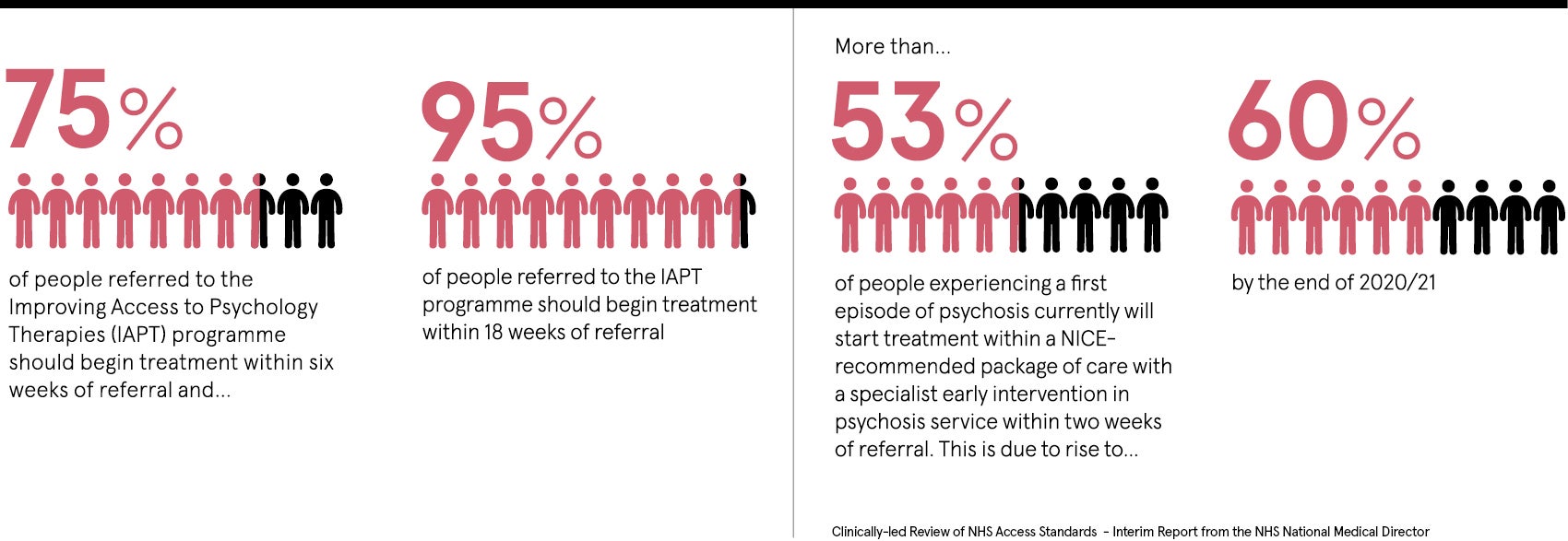
Patients currently face long waiting lists
Currently patients with serious mental health issues, leading them to self-harm or attempt suicide, are being left to wait as long as two years for specialist support. GPs and community health professionals do what they can to support mental health patients on waiting lists, but many patients come to harm and need emergency treatment in A&E.
When patients are finally admitted to an appropriate care facility, the demand for beds, limited budgets and an NHS target-driven culture means they are often discharged long before treatment has been effective and they are ready to go home.
Consequently, patients find themselves virtually abandoned in their communities, struggling to survive before eventually being readmitted to hospital. So, it continues, and each time the patient becomes more vulnerable and the prospect of recovery more distant.
Lack of community-based support is a serious issue
Patients are at increased risk after they have been discharged from hospital, yet the support available to them is poor. A report by the mental health charity Mind confirms what we know from our own experience that NHS mental health teams do not check up on vulnerable people after their discharge, as required by the National Institute for Health and Care Excellence, within one week.
Patients should only be discharged from specialist mental health services when there are ongoing care arrangements in place for them. Failure to do so can put the patient at risk of harm, their condition can relapse and it can mean they are more likely to go back into hospital.
This revolving-door approach is failing patients and their loved ones. It also comes at huge, avoidable cost to taxpayers, at a time when the NHS is under intense pressure to make best use of every pound spent to ensure its long-term sustainability.
We need to treat the underlying causes
At Cygnet Health Care we know that the most effective response to mental illness is to treat the underlying causes and this takes time. There is no quick fix for patients with acute mental illness. We have developed an array of services for patients with mental health needs, and have built a reputation for delivering pioneering services and outstanding outcomes for the people in our care.
We have more than 150 centres across the UK, with over 1,000 beds. Our national network of services provides treatment, care and rehabilitation for men and women, including specialist services that provide low or medium security for individuals with personality disorder, autistic spectrum disorder or who are deaf.
We are very proud that the Care Quality Commission (CQC) has just rated the care provided by three of our hospitals; Cygnet Cedars and Sherwood Lodge — Cygnet’s specialist learning disability hospitals, and Sherwood House, Cygnet’s specialist rehabilitation mental health hospital — as ‘outstanding’.
Cygnet Sherwood Lodge achieved the extraordinary accolade of being rated as outstanding across all five of the CQC’s assessment categories for caring, safe, effective, responsive and well-led services, and it joins Cygnet Elms as the second of only two learning disability hospitals in the country to have achieved this extremely rare honour.
We provide safe and comfortable mental health rehabilitation environments to help people rebuild their life and vocational skills, ready to regain their place in the community. Our low and medium-secure services are focused on therapy and recovery, with the aim to progress service users into the least restrictive environment possible.
Our range of emergency and rapid access services for adults include hospitals that can provide psychiatric intensive care units, acute wards, older adult-specific services and those for people with a learning disability. We offer a national network of more than 200 beds to meet the acute needs of people requiring a rapid admission to mental health services, including those who may need an intensive care environment.
We work closely with NHS England, NHS Wales, clinical commissioning groups, NHS provider trusts, other NHS authorities, local authorities, and individuals and their families to create and provide packages of treatment, rehabilitation and care that give the best possible chance of positive outcomes.
Driving quality healthcare is our priority
Cygnet continually works to improve the quality of treatment for those who use our services. We aim always to have people at the centre of their care and to keep our standards high.
We support these commitments with high standards of staffing, including a continuous programme of learning and development for all employees, evidence-based training and regular staff appraisals, alongside a high staff-to-service-user ratio enabling individual care. We make sure there is always an appropriately qualified consultant doctor available.
Service users are encouraged and supported to be involved in the day-to-day running of each service, which helps us ensure the correct high standards of accommodation, catering, therapy and activities are provided. There is a comprehensive daily therapy and activity programme created by specialist staff and available to all patients.
We are committed to maintaining national good practice standards and are members of quality review forums such as QNIC (Quality Network for Inpatient CAMHS or child and adolescent mental health services) and The Quality Network, and are monitored by the Care Quality Commission.
By monitoring policies and procedures regularly, we make sure they are in line with up-to-date professional guidelines and proven good practice. We also arrange independent audits of our clinical care and management systems, and make the reports available to all relevant bodies.
At Cygnet we share society’s aspiration for all people with mental health issues to live their lives in the community as fully as possible. We believe that to end the revolving-door approach to mental health, the best way is to put the person first, not the condition, and ensure the fullest range of options for care is available to all.
For more information please visit www.cygnethealth.co.uk