Relatives can struggle with lack of information, but filling this void with good communication and greater awareness can help to reduce mental health relapse rates and deflect stress for families.
Cygnet Health Care, one of the UK’s leading independent providers of mental health services, believes more can be done to support families when a loved one is preparing to return to the community.
“Empowering relatives is a massive piece of the jigsaw that is sometimes missing,” says Dr Tony Romero, Cygnet’s chief executive. “They should be part of the solution.
“Collectively, across hospitals and services, more can be done to help prepare individuals and their families for discharge, which would serve to reduce the cycle of relapses that can affect significant numbers of people during the course of their lives. Involving relatives more can help to improve the recovery process.”
The need is pressing as the Mental Health Foundation has predicted that, due to population growth, by 2030 approximately two million more adults in the UK will have mental health problems.
Depression is predicted to become the second leading cause of global disability this year while the London School of Economics and Political Science recently estimated that just a quarter of people with mental health problems currently receive any treatment.
“These figures are daunting, but a lot of problems can be addressed if we adopt a different approach,” says Romero. “One of the key issues is what support and knowledge we give individuals and their families, not only during their treatment, but also to help them when a loved one returns home. 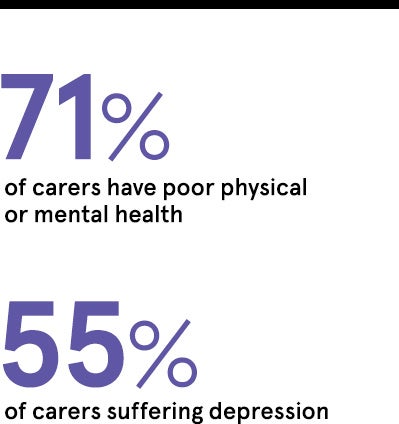
“If you have a fractured hip, you get crutches, physiotherapy and advice on how to make the best of your condition. If your child bumps their head, you get sent home with information telling you what to watch out for. If you are caring for a loved one who has had surgery, the community nurse will show you how to change a dressing.
“We need to replicate this approach in mental health. Currently, there is a lot of training and support available for a physical illness, but not for a mental health condition.
“We need to change this and give relatives a sense of ownership, so they can tell how well they are doing. Information and guidance can be so vital for their ability to care while also reducing their anxiety.”
Looking after a family member with a mental health problem can have a devastating impact on the carer’s own mental wellbeing. The Mental Health Foundation reported that 71 per cent of carers have poor physical or mental health. Stress is common with 55 per cent of carers suffering depression, according to the charity Carers UK.
Parity of esteem, the principle of giving mental health equal priority to physical health, was enshrined in the UK in 2012, but this laudable aim still requires more attention in this area. Cygnet Health Care believes there is a need for an innovative approach to care and aftercare that involves families more.
It is already building in greater involvement by deploying parent liaison support roles and through the establishment of people’s councils across its services to allow voices and concerns to be heard and have a real influence on service delivery.
“The ripple effect of mental illness can keep going if we don’t do enough to support carers,” says Romero. “But the ripple effect can work in a positive way as our everyday skills and compassion can put families at ease through good communication and information-sharing. We’re not just helping one person; we are helping those around them too.
“Our experience has shown it works. The parent liaison role was introduced at our CAMHS [child and adolescent mental health services] as a result of direct feedback. When a loved one is being cared for away from home, feelings are already heightened and there are all kinds of mixed emotions for families. By providing a regular point of contact, concerns and frustrations can be discussed and we have seen a reduction in complaints.
“By collaborating across the mental health sector we can make sure we are providing the additional human touch for families. Too often, anxious parents end up going to the GP, their other children can suffer, then the parent feels even worse. It is a vicious cycle.
“But simple interventions can reduce stress. Doing more to communicate pays dividends by empowering relatives and stopping them feeling helpless and guilty; all they want to do is help.”
Cygnet is trialling more family involvement initiatives and hopes its experiences will have a significant impact on the holistic support and wellbeing of individuals and their families.
“We are happy to share our findings with the NHS and work together with other providers because this is definitely something we need to discuss at a national level,” Romero concludes.
For more information please visit cygnethealth.co.uk

