The UK may have been the birthplace of in vitro fertilisation (IVF), but cuts to NHS fertility services have led some people to consider travelling across the globe for fertility treatment.
The National Institute for Health and Care Excellence recommends three cycles of IVF for those who are eligible, but whether you get anything approaching this depends entirely on where you live.
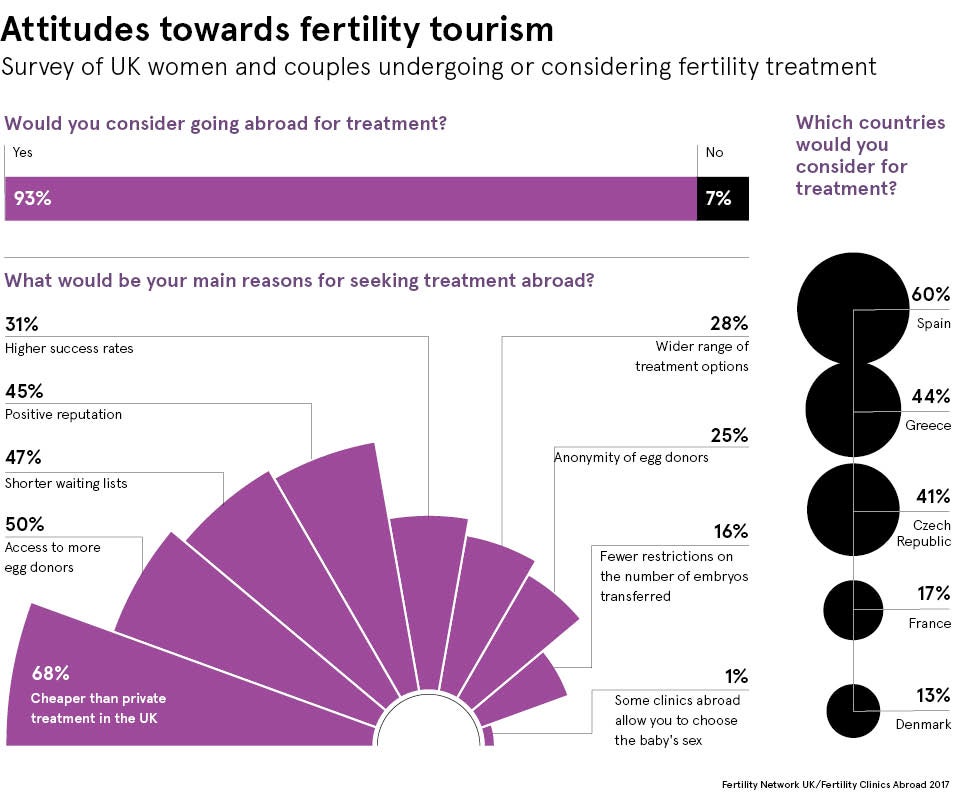
A survey carried out by Fertility Network UK and Fertility Clinics Abroad found that patchy NHS provision and the high cost of private IVF were the main drivers for people travelling overseas. Spain, Greece, Cyprus and Eastern Europe are all popular, along with destinations further afield such as the Caribbean.
IVF treatment overseas may look much cheaper, but headline prices on clinic websites are only part of the picture. The cost of drugs, scans, blood tests and specialist medical insurance are rarely included and can quickly mount up. There is also travel and accommodation to factor into the budget, as well as living expenses abroad.
It is not just cost, but also success rates which can tempt people to travel overseas and half the respondents to the Fertility Network UK and Fertility Clinics Abroad survey believed overseas clinics were more successful.
It is worth noting that the high success rates quoted on clinic websites are often pregnancies rather than live births which are not comparable. Also clinics can be selective about their figures by excluding older patients or selecting a short period when success rates were unusually high.
In the UK, the Human Fertilisation and Embryology Authority, which regulates fertility clinics, gives verified success rates for every licensed clinic, but there is not the same verification process overseas. If you see a figure which appears to be completely out of line with anything you have come across elsewhere, caution is advisable.
One of the reasons people started travelling overseas for fertility treatment was to access donor eggs and sperm. In the past, there were long waiting times for donor eggs and overseas clinics could offer a quick route to treatment. Now many UK clinics have donor eggs available and most can access donor sperm, although this may be imported.
The way donors are recruited, screened and counselled is also something worth checking. In the UK, people conceived using donor eggs and sperm can find out about their donor once they are 18, but some countries only allow anonymous donations, so nothing will be known about the donor.
Nina Barnsley, director of the Donor Conception Network, says it is important not to forget the impact this may have. “We need to keep in mind that if treatment is successful, this new child will have their own thoughts and feelings. Keeping doors open for them in terms of access to information about the donor and/or half-siblings might be really important in the future.”
It has been recognised, in the UK, that multiple births are the biggest risk from IVF to both babies and their mothers, and it is best practice for women to have a single embryo transferred where appropriate. Some overseas clinics do not take the same approach and regularly put back multiple embryos in women most likely to get pregnant with more than one baby.
There is a well-regulated system in the UK where clinics have to meet certain standards and are regularly inspected, but this is not replicated elsewhere
Jane Denton, director of the Multiple Births Foundation, says this is a real concern. “Miscarriage, high blood pressure and pre-eclampsia, haemorrhage and caesarean sections are more common in multiple pregnancies putting mothers at greater risk,” she says. “The babies are much more likely to be born prematurely so more die, and have disabilities and long-term health problems. Having one child at a time is much safer for mothers and babies.”
There is a well-regulated system in the UK where clinics have to meet certain standards and are regularly inspected, but this is not replicated elsewhere. It is, therefore, important to check the rules and regulations, and also the legal situation if you are using an overseas donor or a surrogate.
In addition, there are practical issues to consider, such as potential language barriers, as it can be difficult to talk to a doctor through a translator and it is advisable to check how communications with the clinic are handled.
The key piece of advice to anyone thinking of travelling for treatment is to do your homework before making any decisions. Fertility treatment always involves a significant financial and emotional investment, and making sure you are happy with the clinic you choose will lead to a more positive experience, whatever the outcome.