
At the same time, investors, employees and customers are now looking beyond traditional measures of corporate success, placing increased emphasis on issues of sustainability, ethics and social responsibility.
As global enforcement of regulations increases, punitive fines continue to swell and public demand for ethical business grows, the question of whether to develop an integrated ethics and compliance programme is an easy one to answer.
In short, it’s not a question; it’s an imperative strategic decision that offers numerous benefits: a better reputation, greater transparency, a stronger legal defence, more robust processes and better use of data, for starters.
Yet we are navigating strange and challenging times, and implementing an ethics and compliance programme can be an intimidating, if not overwhelming, experience – especially if starting from scratch.
“The coronavirus pandemic has helped to build a strong case for compliance and ethics,” says Vera Cherepanova, ethics and compliance consultant at Studio Etica and the lead author of NAVEX Global’s Definitive Guide to Ethics and Compliance. “Our wellbeing, and the wellbeing of others, depends on how compliant we all are. In the same way, the wellbeing of organisations depends on our individual and collective conduct.”
Ahead of the launch of the new guide, which will help organisations develop and implement their own ethics and compliance programme, here are the six key steps to consider as you pursue your own plan.
How telemedicine can help
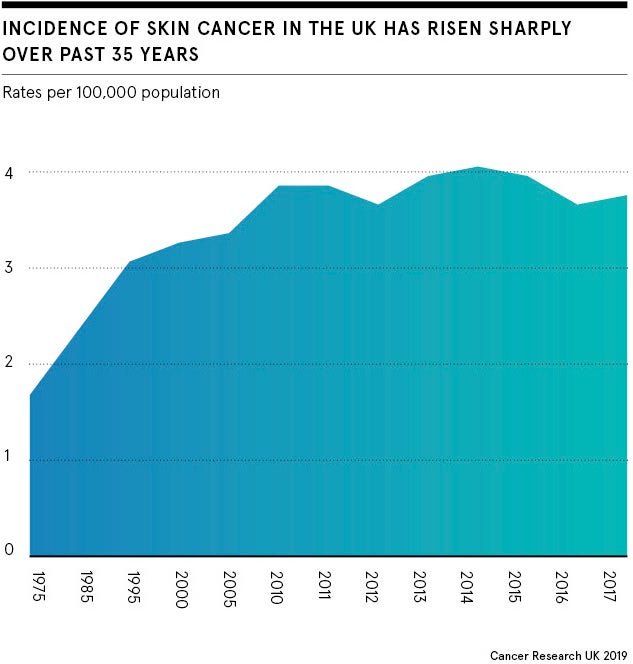
Telemedicine has been hailed as a solution. Skin diagnosis and monitoring apps, such as Skin Analytics, Miiskin or MoleCare, present an opportunity to clear the backlog of patients created by the pandemic and could make it possible to catch additional skin cancers early on.
Neil Daly, chief executive of Skin Analytics, believes there is “no answer that doesn’t involve technology like ours”. He says: “We just don’t have the resources to cope with the number of patients otherwise.”
The rise in commercial skin diagnosis apps could reflect an increased desire for patients to take healthcare into their own hands, especially in light of COVID-19. “It’s empowering for the patient because it enables them to take control of their own health,” says Dr Sharon Wong, dermatologist based at London Bridge Hospital.
However, there are concerns about unregulated commercial apps diagnosing and treating skin cancers and skin conditions.
As dermatologists we will and we should move along with how technology develops. AI will be the way forward and we do need to adapt our ways accordingly
John Loder, investment director for Nesta, an innovation foundation, is optimistic about the potential of sophisticated telemedicine technology, but says it must be properly regulated and tested in clinical settings. “The regulatory environment is not completely nailed down,” he says.
A BMJ report released in February looked into publicly available skinScan and SkinVision apps, and concluded algorithm-based smartphone apps had a “poor and variable performance”, saying “these apps have not yet shown sufficient promise to recommend their use”.
Challenges with app-based healthcare services
If telemedicine solutions don’t have a high degree of accuracy they could cause additional problems, such as missing cancers and offering false reassurance or further overloading healthcare professionals.
“If a patient goes to a GP and says this app says this, it’ll be difficult for the GP, who is not a skin expert, to disagree. So we could get more patients referred to the dermatologist, which could even increase the workload,” says Dr Adil Sheraz, consultant dermatologist and British Skin Foundation spokesman.
On top of this, images patients take themselves on smartphones might not be clear, so apps could miss problems.
Another concern is that a lot of the images in app databases are from lighter skin types. “So they could widen the gap we already have in picking up melanomas in darker skin types,” says Sheraz. “We have to be careful to cater for all different types of skin cancers.”
Where it’s used, telemedicine works best alongside healthcare professionals. One reason for this is the emotional element of diagnosing cancer and need to reassure patients, says Daly at Skin Analytics. “People are really complex and AI is a blunt tool that you need to target in the right way,” he says.
For example, Wong says if a patient of hers had a lesion that looked concerning, she could prime them for the possibility of bad news early on.
Dermatologists can also examine patients physically. “Ultimately humans will prefer to have human interaction and AI isn’t able to engage in that higher-level conversation,” she says. “As a human we can examine not just on a visual aspect, but also on a tactile aspect. We can touch the skin.”
Health services of the future
Despite the misgivings, many in public healthcare and digital health are excited about the possibility of telemedicine and envision a future where skin diagnosis apps work alongside clinicians.
Digital solutions can reach remote locations and people unable to access services due to the coronavirus pandemic. Both Wong and Sheraz say they believe skin monitoring apps, such as Miiskin, are already helpful and would like to work with more regulated, sophisticated digital tools in the future.
“As dermatologists we will and we should move along with how technology develops. AI will be the way forward and we do need to adapt our ways accordingly,” says Sheraz. “I’m really happy people are looking at this technology.”
Wong agrees. “During COVID we’ve used teledermatology a lot and it’s only pushed to the forefront the importance of embracing and working alongside technology to improve patient care,” she says.
Telemedicine has the potential to streamline healthcare services and help dermatologists to detect skin cancers. But there are still a number of challenges that must be overcome to ensure the range of skin diagnosis apps are regulated, sophisticated and safe to use.

At the same time, investors, employees and customers are now looking beyond traditional measures of corporate success, placing increased emphasis on issues of sustainability, ethics and social responsibility.
As global enforcement of regulations increases, punitive fines continue to swell and public demand for ethical business grows, the question of whether to develop an integrated ethics and compliance programme is an easy one to answer.





